Specialized Intra-Articular Injections – PRP
The use of substances derived from a patient’s own blood has been employed in medicine for many years. In these therapies, a small amount of blood is taken from a vein in the patient’s arm, processed, and then re-injected into the body—for example, into a joint affected by osteoarthritis or into an injured tendon. Treatment with autologous platelet-rich plasma (A-PRP) is a specialized form of this method, in which mainly the blood platelets are used to support the body’s natural healing processes.
By the end of the 20th century, the first attempts were made to produce platelet-rich plasma from centrifuged autologous blood. Today, autologous blood therapy is used to promote healing of open wounds as well as in cardiac and thoracic surgery, dentistry, and plastic surgery. Another important area of application is joint treatment. This method has been shown to be effective for cartilage damage (osteoarthritis), tendon or ligament injuries, muscle strains, and soft tissue inflammation, such as bursitis or tendinitis.
Function of Platelets in Autologous Blood Therapy
Platelets (or thrombocytes) are produced in the bone marrow and are responsible for blood clotting. This essential mechanism allows the body to stop bleeding and repair wounds.
When a blood vessel is injured, platelets gather at the site of damage and stick together, forming a small clot that closes the wound and stops the bleeding. At the same time, they release hormone-like substances called growth factors, which help the healing process. Additionally, they attract stem cells, which can differentiate into various tissue types. These cells are essential for regeneration and repair of damaged tissue.
Role of Blood Plasma
Blood plasma is the liquid component of blood, making up about 55% of the total blood volume. Its primary role is to transport blood cells and nutrients through the body’s vessels.
In addition to plasma, blood contains cellular components, known as the hematocrit. These include mainly red blood cells (erythrocytes), which make up about 99% of the hematocrit and are responsible for oxygen transport. Other cellular components include white blood cells (leukocytes), which protect the body from infections, and platelets (thrombocytes), which are important for blood clotting.
What is Autologous Platelet-Rich Plasma (A-PRP)?
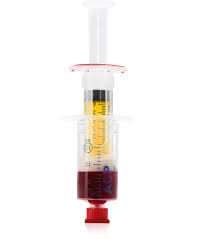
Autologous platelet-rich plasma (A-PRP) is a platelet concentrate derived from the patient’s own blood. It contains blood plasma, from which most red and white blood cells have been removed.
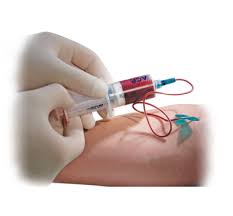
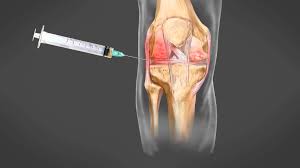
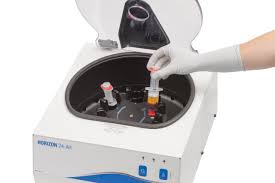
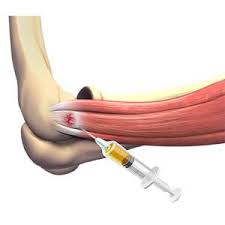
To prepare A-PRP, a small amount of blood is drawn from the patient’s arm vein using a syringe. The blood is then placed in a centrifuge, which separates the plasma from the other cellular components. This process is called plasmapheresis.
When this platelet-rich plasma is injected into the site of injury or inflammation, it supports the body’s natural healing processes and contributes to tissue regeneration, such as cartilage or tendons.
The exact mechanism of action is not yet fully understood. However, it is believed that substances in the plasma—such as growth factors, interleukins, and the platelets themselves—activate and support healing in inflamed tissues. Platelets also appear to help form new connective tissue, reduce inflammation, and protect cartilage.
Because each person has a different blood composition and internal environment, the results of A-PRP treatment may vary from patient to patient. Allergic reactions or immune problems do not occur, as only the patient’s own material is used.
Applications of A-PRP Therapy
A-PRP therapy is used for many musculoskeletal conditions, affecting joints, muscles, tendons, and ligaments.
Common indications include:
- Osteoarthritis (joint wear) and arthritis (joint inflammation)
- Soft tissue inflammation, such as tenosynovitis
- Muscle strains and fiber tears
- Complete or partial ligament tears
- Tendinitis, such as Achillodynia (inflammation of the Achilles tendon)
- Intervertebral disc herniation (disc disease)
- Rotator cuff injuries of the shoulder
- Support of wound healing after surgeries, such as arthroscopy
A-PRP therapy can accelerate healing, reduce inflammation, and support natural tissue regeneration.
Treatment of Osteoarthritis with A-PRP
Osteoarthritis is a joint disease caused by the degeneration of articular cartilage. Cartilage acts as a “cushion” and protects bones inside the joint from friction.As cartilage begins to wear down, this protection decreases. Over time, with progressive cartilage loss, the bones come closer together and rub against each other, causing pain, swelling, and reduced joint mobility.
The joints most commonly affected are the knee and hip, as they bear the most body weight.
Why is A-PRP an Alternative to Other Osteoarthritis Therapies?
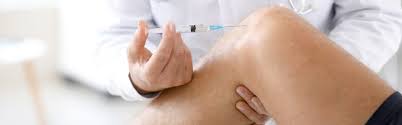
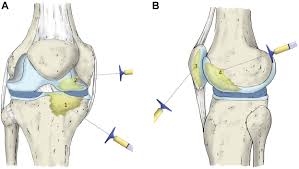
The goal of autologous platelet-rich plasma (A-PRP) therapy is to reduce pain and improve joint mobility. The platelet-rich plasma comes from the patient’s own blood. The doctor injects this concentrate directly into the joint to activate natural cartilage regeneration.Typically, multiple sessions of A-PRP are needed to achieve noticeable results.
Studies have shown that A-PRP injections in knee osteoarthritis provide significantly greater pain relief over 12 months compared with saline injections (Görmeli et al., 2014).
Unlike cortisone injections, which can damage tissue and cause connective tissue atrophy, A-PRP therapy is considered a gentle and natural method, as it modulates inflammation without destroying tissue.
Additionally, A-PRP does not have the serious side effects that NSAIDs can cause, such as stomach irritation or damage.
Many studies also show that A-PRP injections have equal or better effectiveness than hyaluronic acid injections in patients with knee osteoarthritis.
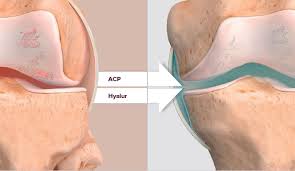
The active substances and growth factors in platelet-rich plasma that help protect and repair cartilage include:
- Growth factors from platelets stimulate growth and proliferation of cartilage cells (chondrocytes)
- Clotting factors and cytokines enhance new cartilage formation
- Clotting factors inhibit the action of inflammatory substances that break down cartilage
- Growth factors such as TGF-β, IGF-1, BMP, PDGF, and VEGF support the development, maturation, and nutrition of cartilage cells
- Production of type II collagen, an essential cartilage component, is promoted
- Inflammation in active arthritis is reduced or stopped
- Production of the lubricating protein Lubricin (Proteoglycan-4) is enhanced, protecting and stabilizing cartilage
Compared with hyaluronic acid injections, A-PRP therapy is considered more effective, especially in patients with early-stage osteoarthritis, as it significantly improves pain and joint mobility.
Consult our clinic to find out if this therapy is suitable for your condition.